
Cancer poses a rising threat to global health as well as the world economy. International experts have agreed on a strategy that can meet the challenge. They are now calling on world leaders to wake up to their responsibilities and act.
It’s official. Non-communicable diseases now account for two out of every three deaths worldwide – a massive turnaround from twenty years ago, when they were outnumbered two to one by deaths from communicable, maternal, neonatal and nutritional causes. This is one of the headline findings of the Global Burden of Disease study, published in The Lancet, December 2012. Around eight million people now die of cancer every year, a rise of almost 40% over the past 20 years. This means that cancer is not only one of the biggest global killers alongside cardiovascular diseases, but also one of the fastest growing causes of death. The WHO predicts that by 2030, 22 million men women and children will be diagnosed with cancer every year, and 13 million will die of the disease.
This humanitarian disaster has knock-on effects that extend well beyond those directly affected. A study by the American Cancer Society and the Livestrong foundation has found that, leaving aside the direct costs of treatment, the economic impact of premature death and disability from cancer drains $900 billion a year from the world economy – around 1.5% of global GDP (figures for 2008).
Members of the cancer community are not surprised by these statistics, which confirm trends that have been documented for many years. They are, however, increasingly alarmed at the apparent lack of response among national and global leaders to what is unquestionably an escalating crisis.
Where, they ask, is the sense of urgency that forced the AIDS epidemic on to the agenda of G8 summits? Where is the momentum and drive for the sort of collaborative effort that is providing some of the poorest communities in the world with access to affordable anti-retroviral drugs and developing and strengthening networks of community-based health professionals to deliver care and prevention programmes? Who will take a lead on tackling cancer, and when?
In an effort to build a high-level consensus around such an effort, the European School of Oncology invited leading international experts working on every aspect of cancer, and from all corners of the globe, to a World Oncology Forum in Lugano in October 2012. Their task was to address the question: Are we winning the war on cancer?… and to draw up a battle plan to get the job done.
This unusual and intriguing gathering had experts who straddle clinical and scientific research sitting alongside specialists in cancer epidemiology, prevention, health policy, advocacy and policy implementation, to make a critical assessment of whether their collective efforts are on track – and what needs to happen to turn the tide against cancer.
To ensure that this assessment reflected major regional disparities in the disease burden, and potential solutions, the discussion included experts not just from North America, Europe and Australia, but also from Asia (India, Japan, Korea and China), South and Central America and the Middle East.
A group of health journalists from across the world were invited to play ‘devil’s advocates’ – to subject the whole conversation to the scrutiny of outsiders and ask awkward questions. Two additional outsiders also played a critical role. Rifat Atun, who spent many years working for the Global Fund to Fight AIDS, Tuberculosis and Malaria, led a discussion on what the international efforts against cancer could learn from that experience. Richard Horton, editor of The Lancet, was there to ensure that the Forum was more than a talking shop, challenging it to come up with a strategy that works within the context of the wider global health and development agenda, is simple enough to sell to busy people with packed agendas, yet is bold enough to turn the tide on cancer.
Though it was organised with policy makers in mind, the World Oncology Forum was not stage-managed and there was no cheerleading. It was an honest exercise in examining the evidence to ensure that any plan that emerged could command confidence.
Winning or losing?
The evidence on the alarming rate of increase in new cases and deaths tells a clear story: we are failing to control cancer. And this generated the most important message from the Forum: Current strategies are not working; carrying on business as usual is unthinkable; new strategies are urgently needed.
Carrying on business as usual is unthinkable; new strategies are needed
Behind the stark headline figures, however, a more complex picture shows important progress in some areas.
Cancer is becoming more common everywhere in the world. In the developed world we are getting fatter, exercising less, eating less healthily and drinking more alcohol – all of which are independent risk factors for cancer. But while the number of new cases is rising, the number of people dying from cancer is slowly falling.
In low- and middle-income countries, the rate of new cancers is increasing even more quickly, as higher living standards enable people to adopt ‘western lifestyles’ – not least smoking – and fewer people die young from infectious diseases. In these countries the rise in new cases of cancer is leading to a similar rise in the numbers of deaths.
The lessons of falling mortality
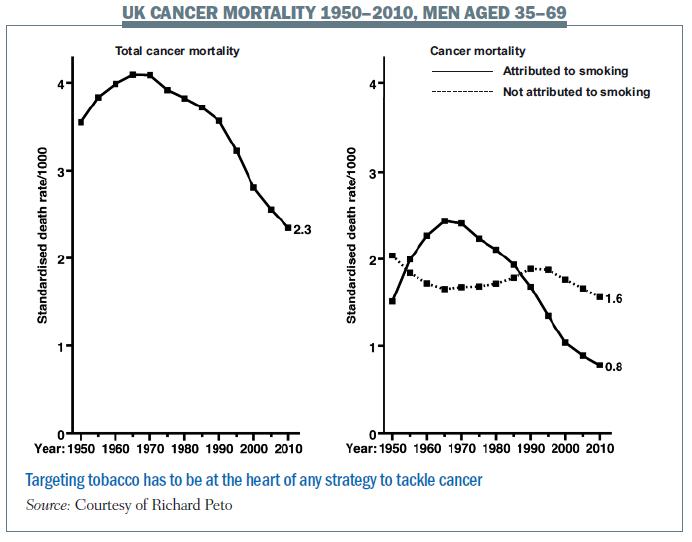
Richard Peto, professor of medical statistics and epidemiology at the University of Oxford, drew the lessons from 60 years of falling mortality trends for the UK, focusing on men in the 35–69 age group. His graphs told a story that came as quite a shock even to this hardened group of cancer professionals. In 1965 smoking-related cancers accounted for more deaths than all other cancers put together. It is the drop in deaths from smoking-related cancers – from more than 250 per 100,000 in 1965 to around 80 per 100,000 in 2010 – that accounts for almost all the improvement in cancer mortality rates. By contrast, the risk of dying from other types of cancer has changed relatively little in this population – rates in 2010 were similar to the 1960s, though they have been on a slow downward trend over the past 20 years thanks largely to better treatment for colorectal cancer and an unexplained drop in incidence of stomach cancer.
The drop in deaths from smoking-related cancers accounts for almost all the improvement in UK male mortality rates
The close link between tobacco and cancer comes as no surprise, given that it plays a role in a wide variety of cancers and causes 90% of lung cancers. However, many participants at the Forum were shocked to see how much of the total burden of cancer is caused by this one industry, and how effective anti-tobacco measures have been in relation to other strategies for cutting cancer deaths. More shocking still were the figures Peto gave for the escalation in rates of smoking across the globe, which accounts for a major part of the explosion in new cancer cases: every year 30 million people are taking up smoking – 50% of young men and 10% of young women. India is already seeing 1 million smoking-related deaths every year. In China smoking-related deaths are expected to triple in the next two decades, killing some 3.5 million people annually by 2030.
Forum participants agreed that any strategy for turning the tide against cancer needs to rapidly reverse this rise in smoking – in the words of one participant, “We need to stop pussyfooting around tobacco.” Taxing sales has been shown to be effective up to a point. Experience has shown that tripling the price of tobacco roughly halves consumption and doubles tax revenues – though beyond a certain price the policy is undermined by large-scale smuggling. Far more effective would be to deter investors, through a global agreement to tax the profits of tobacco companies. This single measure could do more to turn the tide on cancer than anything else.
Invest in prevention
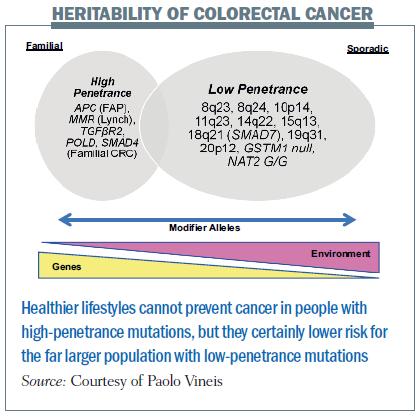
Paolo Vineis, Chair in Environmental Epidemiology at Imperial College, London, looked at the evidence on what causes cancer and what can be done to prevent it. What is becoming clear, he said, is that cancers are caused by an interaction between hereditary (genetic) and environmental/lifestyle factors. Heredity plays the overwhelming role in a few cancers, such as familial adenomatous polyposis – children who inherit the mutated APC gene invariably go on to develop this cancer. In other cancers, environmental exposure is more important, with genetic susceptibility playing a more minor role. Most cancers lie somewhere along this spectrum, with environmental and lifestyle factors interacting with genetic susceptibility.
It is the increase in environmental and, above all, lifestyle risk factors that are the major driver behind the escalation in the number of new cancer cases across the globe (together with increases in life expectancy in the developing world). There is evidence to show that, in richer countries like the UK, up to 45% of cancers in men and 40% in women could have been prevented had risk factors such a tobacco, alcohol, lack of exercise and overweight, been reduced to optimal levels (Br J Cancer 105:S77–S81). At a world level, the Global Burden of Disease study shows that eating too much of the wrong stuff has overtaken malnutrition as a risk factor for death, not just from cancer but from a variety of chronic diseases.
While this opens important possibilities for cancer prevention, participants at the Forum cautioned that it is very hard to convince people to change to healthier lifestyles, particularly when ‘cancer causing industries’ are employing the best brains and huge marketing budgets to encourage them to increase their risky behaviour. Proper funding combined with an evidence-based approach will be needed, drawing on what has been shown to work elsewhere and adapting it to local cultures and demographics. This will require a major shift in government priorities, warned Vineis, who pointed out that in the US, Canada and Europe less than 4% of public funding of cancer research is currently spent on prevention, and that the growing trend towards privatising parts of healthcare systems is likely to impact on preventive activities such as health promotion, which are not appealing for private enterprises.
Cancers caused by infectious diseases, particularly liver and cervical cancer, also offer huge opportunities for prevention, said Vineis. Liver cancer is one of the top three – and fastest rising – causes of cancer death for men in much of the developing world, with a sizeable majority originating in hepatitis B infection, for which vaccines are available that have proved their worth in a variety of developing country settings (other causes include hepatitis C and alcohol). Cervical cancer is one of the top causes of cancer death in women in much of the developing world, and can be controlled though HPV vaccination programmes, or even low-tech screening programmes. Both these cancers are particularly devastating as they have a relatively young age profile, depriving families of mothers and providers. Participants agreed that rolling out prevention programmes, within a short timeframe, to all communities at risk, has to be a key part of any strategy to prevent cancer.
 Collaborate for a cure
Collaborate for a cure
Prevention is better than a cure – and nowhere is that more true than in cancer. However, even under optimal levels of risk reduction, the majority of cancers are not preventable. We need a cure. Douglas Hanahan of the Swiss Institute for Experimental Cancer Research, in Lausanne, presented the evidence on how well the battle plan to find one is working. “Not very well,” was his verdict.
Hanahan is known for characterising the ‘acquired functional capabilities’ of cancer cells, coining the phrase the ‘hallmarks of cancer’. These include the ability to invade tissue and metastasise, evade growth suppressors, resist cell death and avoid immune destruction. The problem with the new generation of targeted drugs, he said, is that while they have been successful at ‘taking out’ one or maybe two of these functional capabilities, they are not attacking them all. This explains what we have been seeing, for instance, after treatment with angiogenesis inhibitors, or BRAF inhibitors in melanoma: dramatic impact on cancer in a matter of weeks, followed by an aggressive return of the disease. The stream of new cancer therapies are, with few exceptions, failing to deliver the major benefits needed, said Hanahan. He suggested that hitting targets harder and targeting several ‘capabilities’ at once could be a way forward.
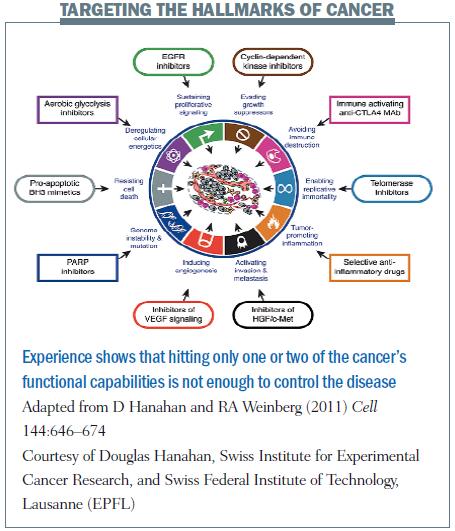
Not everyone at the Forum was convinced. Doesn’t hitting targets harder (with all that implies for accompanying toxicity), and hitting multiple targets, sound a bit like a return to the chemotherapy carpet bombing approach? Given the way tumour cells mutate, shouldn’t we expect that if we target and shut down one mutation the cancer will simply find other mutations to exploit to keep going? Before investing billions on drugs targeted at one mutation after another, shouldn’t we start by trying to understand basic principles of cell behaviour, so we can anticipate the cancer cells’ evasive strategies, and devise rational counterstrategies, based on rigorous mathematical models, to cut off their options?
A broad consensus emerged on one point, however: current models for developing new therapies are not working. They are delivering too little benefit at too great a cost. New ways of collaborating will be needed to deliver therapies that can really transform the prospects of cancer patients the world over.
New ways of collaborating will be needed to deliver therapies that really transform the prospects of patients
The scale and the breadth of collaboration that is needed was nicely demonstrated by Hanahan in the form of a graphic presentation of his “war room” – a new cancer centre in Lausanne involving a partnership of three institutions, designed to foster “synergistic interactions” between knowledge-driven basic scientists, clinical and surgical oncology researchers, bioengineers, pharmaceutical chemists, and clinical specialists in treating cancer patients.
As this type of work can only thrive in a publicly funded academic setting, new models of public–private cooperation will be needed, and governments, regulators, reimbursement authorities, independent research foundations and charities, international health agencies – and oncology professionals – must all play a role in making this happen.
Quality care
While progress towards a knock-out blow against cancer has been frustratingly slow, cure rates for some of the most common cancers have been improving through a series of small steps. The best treatments for early breast cancer show almost 90% of people surviving for at least five years. Treatment of colorectal cancer has also been steadily improving, with five-year survival pushing above 60% in some places. Under the best conditions, almost 90% of childhood cancers are now curable. More and better palliative care starting at an earlier point is helping people to live with cancer with a good quality of life; to earn their living; to care for their families – and even to live longer.
These types of results, however, are currently achieved for only a minority of people and in a minority of countries. Michel Coleman, professor of Epidemiology and Vital Statistics at the London School of Hygiene and Tropical Medicine, and Felicity Knaul, director of the Harvard Global Equity Initiative, presented evidence about how many lives could be saved and how much suffering avoided if all health services provided universal access to the best quality of care that can be achieved at a sustainable level.
Coleman presented figures from Kentucky, USA, showing that women with private healthcare insurance have a 20% better chance of surviving three years after a breast cancer diagnosis than those on Medicaid, the ‘safety net’ insurance for people on low incomes. Even where insurance coverage or co-payments are not an issue, social deprivation can still reduce chances of survival, as was shown in a UK study of survival rates in rectal cancer (Br J Cancer 2008, 99:S30–S32). In 1996–1999, relative survival rates for men living in areas of highest deprivation were 15% lower than for men from the most affluent areas – and as treatments improve, that gap is getting wider. Understanding and addressing the reasons why people from more deprived backgrounds have poorer survival rates must be a key part of any cancer control strategy.
Important lessons about strategies to beat cancer can also be learnt from looking at differences in survival rates between broadly similar countries. The graph below, which gives five-year survival rates for women diagnosed with breast cancer at two different time points, shows what a difference a well-performing cancer system makes and how concerted efforts to improve results can pay off. In the earlier period, women with breast cancer in Sweden had a 40% better chance of surviving five years than those living in Poland. Over the following decade Poland improved its survival rates by almost 15 percentage points, compared with just over 4 percentage points in Sweden. This graph also shows that there is still plenty of scope for survival rates in the worst performing countries to improve.
This is not all about money – although per capita spend on health does of course play a role. Evidence shows that effective organisation and management are important for getting the best results in cancer. This includes adhering to diagnostic and treatment guidelines, ensuring patients are treated by multidisciplinary teams with expertise in their cancer type, having proper systems in place for monitoring how well different parts of the health system are performing – and of course ensuring that all patients have equal access. 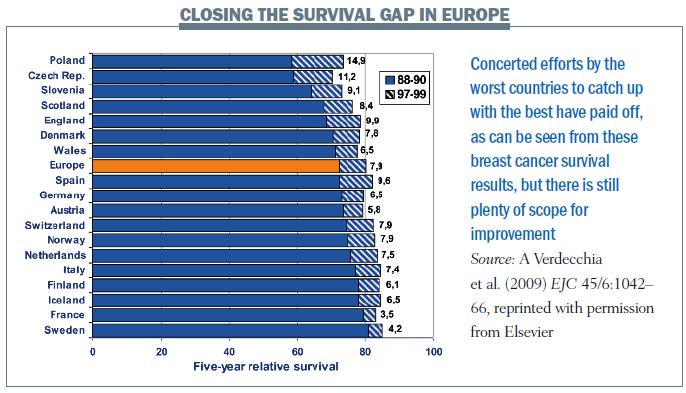
Universal care
Improving the effectiveness of cancer care delivery across Europe and the US will be important, particularly given the current squeeze on public finances. But it is in low- and middle-income countries that the battle to control cancer will be won or lost. These are the countries that are experiencing the biggest explosion of new cases, and they are currently in a poor position to either detect or treat them.
While breast cancer is still far more common in developed countries, most breast cancer deaths are in developing countries; poorer countries also account for 85% of deaths from cervical cancer. Only around 20% of cancer patients survive for more than five years in the Gambia; in Uganda the figure is 13%, except for breast cancer, where five-year survival is around 45%. In the poorest 25 countries, paediatric cancers are fatal in 90% of cases, while almost 90% of children in the richest countries now survive. Lack of pain control and palliative care means that dying from cancer is a far more terrible experience in precisely those regions of the world where death rates are climbing fastest.
Universal access to treatment is one of the big challenges for a global strategy against cancer. Participants at the Forum spoke of the need to challenge widespread fatalistic attitudes based on misconceptions that cancer is simply too complex and too expensive to treat.
Rifat Atun reminded the Forum that similar attitudes were once prevalent about treating AIDS in poor countries, and it took many years of determined advocacy to turn that fatalism around. Once the international aid effort started, and began to show results, attitudes changed. What initiatives like the Global Fund Against AIDS, Malaria and Tuberculosis have shown is that once you have agreement on international action, and are able to pool resources and use a single platform to interact with donors, suppliers, governments and NGOs, what once seemed impossible becomes possible. The prices of essential drugs were slashed – down by as much as 90% in many cases; donations tripled between 2002–2004 and 2008–2010, and many communities are now covered for the first time by primary healthcare networks.
In Ethiopia, more than 30,000 Health Extension Workers were trained and deployed between 2004 and 2009; in Malawi 10,000 Health Surveillance Assistants were deployed by 2009. These people are already acting not just as the frontline for HIV, TB and malaria services, but are also providing community-based maternal and newborn care; family planning advice and disease surveillance. These are the kinds of networks that will be essential for implementing strategies on cancer prevention as well as early detection and some types of palliative care, including pain relief. They will also be important in implementing policies to tackle the stigma and discrimination that can blight the lives of cancer patients and their families. Strengthening and extending these community-based networks, and joining forces with other health and anti-poverty initiatives, will therefore be central to any anti-cancer strategy.
That is not to say that prevention, early detection and palliation is all that people in low- and middle-income countries can expect – indeed early detection is a waste of resources unless the cancers are treated. A key message from the Forum was that many cancers can be treated effectively with basic surgery and radiotherapy facilities, a limited list of essential drugs, and some essential diagnostic equipment, provided the care is planned and carried out by a team of people who specialise in treating those cancers and they have access to evidence-based guidelines on how to deliver the best results with the resources available.
PACT, the International Atomic Energy Authority’s Programme of Action for Cancer Radiotherapy, has long been helping some of the world’s poorest countries establish a radiotherapy capability, and these efforts could be massively expanded within the context of an international strategy against cancer. The Breast Health Global Initiative has pioneered a set of guidelines for early detection, diagnosis and treatment graded accorded to resources. Funding the research needed to develop and implement these sorts of guidelines for other cancers will be an important part of any global cancer strategy.
Important lessons on sustainability can be learnt from Mexico’s universal health insurance programme, Seguro Popular, which started in 2004 and by 2011 had achieved universal coverage for all paediatric cancers, as well as for breast, testicular and prostate cancers and for non-Hodgkin lymphoma. These and other examples indicate that the goal of ensuring that every cancer patient has access to an indispensable package of diagnostics and curative and palliative care is attainable, and this has to be a key element of the international strategy.
The goal of ensuring every patient has access to an indispensable package of diagnostics and care is attainable
An AIDS moment
Opening his presentation on the second day of the conference, Atun commented on a feeling of resignation and lack of ambition he had sensed among participants during the previous day. He had a point. But when Richard Horton introduced the purpose of the Forum – to send an appeal to governments and policy makers to recognise the scale of humanitarian disaster presented by escalating rates of cancer, and to commit to new strategies to meet the challenge – the mood of participants changed from resignation to indignation and determination.
The action plan they came up with is set to be published in The Lancet and leading national and international newspapers across the world, to mark World Cancer Day. The question now becomes how to overcome the fragmentation of the cancer community to build the sort of public, and patient-led movement that proved so effective at forcing global action on AIDS. “We need to go back to basics,” concluded one patient advocate, “we need to mobilise the cancer community, and engage people into forcing governments to act.”
An appeal to world leaders
The World Oncology Forum agreed a 10-point strategy that it believes is achievable and will significantly stem the rising tide of cancer. The aim is to contribute to the goal of cutting premature deaths from non-communicable diseases by 25% by 2025, as agreed by governments at the *World Health Assembly in May 2012, and to reduce the drain on the world economy by addressing one of the biggest causes of premature death and disability.
On World Cancer Day, Monday, 4 February 2013, an appeal will be published in The Lancet and leading national and international newspapers, for policy makers and everyone who can help stop unnecessary deaths from cancer to get behind this strategy.
A 10-point strategy to turn back the tide on cancer
Prevent preventable cancers:
1 Wage war on tobacco, by far the biggest cause of cancer death across the globe. Extend to all countries the anti-tobacco measures already found to be effective and tax the profits made from tobacco.
2 Give people the knowledge they need to understand which cancers threaten them most, and how to reduce their risk; develop and implement scientifically sound strategies, including vaccines, to protect against cancers caused by infections.
Treat treatable cancers:
3 Develop early detection programmes tailored to local needs and resources, which target cancers that are the most detectable and treatable and have the greatest social impact.
4 Ensure that every cancer patient has access to a package of diagnostics and curative and palliative care that has been shown to get the best possible results within the local setting and is delivered by trained health professionals.
Support all those who are living with cancer:
5 Give all patients access to optimal pain control by changing attitudes and removing bureaucratic, legal and logistical barriers to the medical use of morphine.
6 Involve patients as partners in decisions about their own care and give them a voice in decision making about policies that affect them.
Accelerate finding cures for cancers that are not yet curable:
7 Replace the current broken business model for developing new therapies with new and more efficient forms of public–private collaboration, geared to accelerating delivery of affordable therapies that are of real benefit to patients across the world.
To achieve all the above:
8 Educate policy makers and the public to counter the entrenched fatalistic myths and misconceptions that undermine efforts to mobilise forces against cancer and deter people who suspect they may have cancer from seeking early medical advice.
9 Promote and strengthen sustainable and universally accessible health systems that are supported by innovative financing mechanisms, and are driven by evidence about cost-effective ways to deliver the best results and not by vested economic interests.
10 Ensure that all countries have a clear cancer control strategy, that evolves in the light of needs and experience, and is built on creative ideas, backed by solid evidence, in order to turn back the tide on cancer.
* Erratum: The conference at which governments signed up to the target of 25% by 2025 was incorrectly given in the printed version of Cancer World as the 2011 UN Summit, and has been corrected in this online version.






Leave a Reply