
Treating the right patient with the right therapy at the right time depends on having the right picture of every patient’s key biological markers. A number of initiatives are now springing up across Europe to ensure that the testers are indeed getting it right.
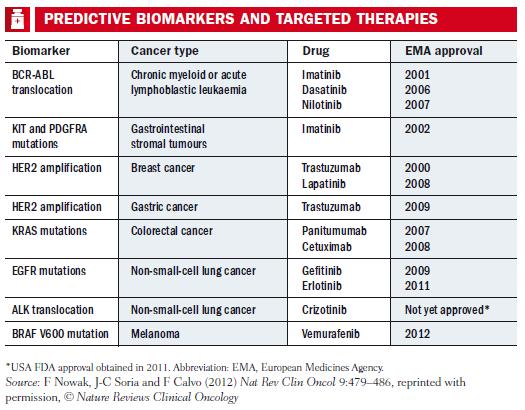
As the era of personalised medicine has developed, it has brought with it the need to conduct an increasing number of biological tests to determine the appropriate personalised therapy. Key examples are HER2 status for response to Herceptin (trastuzumab) and the KRAS mutation, which predicts for a poor response to EGFR inhibitors such as Erbitux (cetuximab).
Now the floodgates are opening, as increasingly sophisticated genetic testing of tumours is revealing a raft of gene mutations, dislocations and fusions that are the target of current or future drugs, notably in lung cancer, where in just a few years possible treatment options have changed dramatically. The sheer number of patients where molecular testing will be essential – such as the many with metastatic colon or lung cancer – is a big challenge now.
Cancer centres are pressing ahead with projects that carry out several assays on tumours to give more information to patients and their oncologists, and to identify people eligible to join clinical trials. At national level in countries such as France and the UK, cancer policy makers are rolling out and making preparations for the routine testing of a range of genetic mutations in the major cancers such as breast, colorectal and lung.
These projects highlight one of the big challenges with molecular biomarkers – ensuring that testing is carried out to a consistently high standard. As Cancer Research UK, which is organising the UK’s Stratified Medicine Programme for a panel of genetic tests, comments about the earlier introduction of Herceptin, “Having to routinely, reliably and accurately test a breast tumour’s HER2 levels, as part of ‘business-as-usual’, was uncharted territory for many pathologists.”
Indeed, Giuseppe Viale, professor of pathology at the University of Milan, has written extensively about controversies in HER2 testing, and has noted that despite decades of experience with assays, and the availability of standardised reagents, kits and guidelines, “the accuracy and reproducibility of the test results are still a major concern worldwide”. Results of several quality-control schemes for pathology laboratories have shown as many as 15–20% false-positives with immunohistochemistry testing, and there can also be a high error rate in another key testing method, fluorescence in situ hybridisation (FISH).
But it is also true that we still don’t understand enough about the biology of breast cancer to be certain about how HER2 testing should best be carried out and interpreted. Tumours are not uniform in biology, and HER2 status may change over time. Uncertainty also remains about the right threshold values for predicting who could benefit from Herceptin. “Many oncologists seem to believe that pathologists are now infallible in assessing HER2 status of breast cancer,” Viale notes, adding that it is frustrating that oncologists are pushing for more precise identification of targets for new agents in breast cancer while basic questions remain about HER2 testing (see Controversies in testing for HER2, ASCO 2011 Educational Book).
“Many oncologists seem to believe that pathologists are now infallible in assessing HER2 status”
KRAS testing
The good news is that tests for other predictive molecular markers do not all suffer from the same complexity. And although quality concerns are still very much to the fore, they have been tackled much more systematically in the case of KRAS, for example, as Han van Krieken, professor of pathology at the Radboud University Nijmegen Medical Centre, explains. “Indeed, HER2 testing is still far from optimal. One important reason lies in the biology. It is not completely known what factor is the most important for predicting trastuzumab response: the amount of protein or the regulation of the expression of the gene or the number of copies of the gene. The other important factor is that early on there was limited interest in the quality aspects. The situation with KRAS is very different: it is clear that activating mutations in the gene are the indicator and within two years of this discovery there was quality assurance.”
KRAS mutations are important, because they occur in around 40% of patients with colorectal cancer, and they prevent EGFR inhibitors such as Erbitux and Vectibix (panitumumab) from working. As the large majority (almost 85%) of patients with colo-rectal cancer have tumours that overexpress EGFR, knowing who will and who will not benefit from an EGFR inhibitor is essential to avoid subjecting large numbers of patients to treatments that won’t do them any good. Guidelines for using EGFR inhibitors therefore advise that testing for EGFR status alone is not enough; you also need to test for a variety of mutations in KRAS.
As van Krieken adds, not all of the 60% who do not have KRAS activating mutations will benefit, and there is not enough evidence yet to further separate out a target group from this majority. “But KRAS testing is common now – I don’t think anyone is giving the anti-EGFR drugs in colo-rectal cancer without it.” What has been critical, he says, is participation in quality assurance programmes at national and international levels, such as the European KRAS EQA (external quality assessment) scheme – a European programme he proposed with colleagues at the European Society of Pathology in 2008, and which is now in its fourth round.
External quality assessment
Elisabeth Dequeker, the KRAS EQA scheme coordinator, who is based at the Biomedical Quality Assurance Research Unit in Leuven, Belgium, says the first step had been a pilot to establish regional laboratories that could prepare slides for the scheme – a quality control exercise in itself. These regional laboratories now send samples for which the KRAS mutation status is known, but not revealed, to laboratories participating in the scheme, to check they are getting accurate results. Between 2009 and 2011, 150 labs in Europe and in countries such as Indonesia and Israel reached a genotyping score of 90% or better in the scheme. “Some countries such as the UK and Germany also have their own national assessment schemes, but most smaller countries do not, and here in Belgium for several years now it is a requirement that all molecular oncology tests must be accredited. The best way of validating tests is with an EQA scheme,” says Dequeker.
Given that there are several ways of testing for KRAS mutations, and also a choice of commercial kits and home-grown systems, the EQA scheme has not attempted to distinguish between approaches. “If you implement your methodology well and validate it according to standards your method will be stable,” she says. “But molecular pathology is not easy and our scheme has found a significant number of errors that could have had a big effect on therapy.”
“Our scheme has found a significant number of errors that could have had a big effect on therapy”
Van Krieken reports that, from the first round of the KRAS EQA scheme, 85% of laboratories had a 100% score on the samples, but 15% still had a substantial number of mistakes. “One mistake is in selection of patient material – you need to have sufficient tumour in your samples, and you may need to enrich them by cutting out normal tissue. The other main problem was in interpretation of results – some labs were making mistakes even using commercial systems and were missing some of the mutations.”
Some labs may have to pull out of molecular testing if they can’t improve, says van Krieken, but the indications are that with the right quality and educational schemes in place there will be few that cannot make the grade. In 2009, the Italian Association of Medical Oncology and the Italian Society of Pathology and Cytopathology ran a KRAS quality scheme similar to the European one. It found that only two participating centres out of 59 failed a 100% pass rate, and those two also failed a retake, being unable to extract enough genomic DNA for the mutational analyses.
The Italian quality scheme sent samples with a particularly high (>70%) content of tumour cells, but the organisers said that the impressive results may also reflect the benefits of an ongoing networking programme (called KRAS aKtive).
Lung cancer mutations
The European Society of Pathology EQA scheme has this year been extended to non-small-cell lung cancer (NSCLC) in two phases, first just the ALK mutation, which has generated much interest in oncology, and then a second round covering ALK, KRAS and EGFR, says Dequeker. France, which has its own quality schemes, is collaborating with Leuven on validating EGFR and BRAF programmes – the latter, for advanced melanoma, is turning out to be quite a challenge.
“What we are finding is that each test has its own problems,” says van Krieken. “For example, the quality of DNA in a skin cancer biopsy can be affected by melanin, and sensitivity issues are very important in lung cancer as samples can be small. Each test and tumour needs its own EQA programme – you cannot assume a lab doing well with KRAS in colon cancer will also do well with say BRAF for melanoma.”
“You cannot assume a lab doing well with KRAS in colon cancer will also do well with BRAF for melanoma”
Rolf Stahel, professor of oncology at Zurich University Hospital, Switzerland, and a lung cancer specialist, comments that the diagnostic possibilities for NSCLC are becoming very complex, although so far only EGFR mutations are recommended for testing at the first-line stage by the ESMO consensus panel on NSCLC pathology and molecular testing, on which he serves. The targeted drugs on offer here are the EGFR blockers Iressa (gefitinib) and Tarceva (erlotinib), with others in the pipeline, and there is a sizeable population – 10–12% of those with NSCLC.
“Now ALK testing is also recommended, but in second-line treatment,” says Stahel. “But here the testing is not easy as we don’t have a final word yet on how best to test for it – will it be FISH, or immunohistochemistry and then FISH, or genetic sequencing. And it is in only about 5% of patients.”
While ALK testing has now moved from the investigational stage into clinical practice, the key drug, Pfizer’s Xalkori (crizotinib), was only recommended to receive conditional approval in Europe a few months ago, with the final decision still pending. Other mutations of interest, such as HER2, ROS1 and RET, are lower still in frequency, at 1–2%. This is now raising questions such as whether to prescreen with a cheap assay and then apply a more precise and expensive test on a subgroup. Stahel adds that testing is a “tremendously fluctuating field” as we move up the hierarchy from looking for single mutations, with traditional immunohistochemistry testing near the bottom, to more sophisticated tests such as FISH, to exome sequencing at the top – and indeed whole genome sequencing ultimately.
“And if we test for a huge string of mutations we may also get results we don’t want to know”
he says. “The pathologists here in Switzerland are gung ho about buying new sequencing machines – but how are we going to cope with the information in the clinic? How do we communicate results that are nothing to do with lung cancer?”
“And if we test for a huge string of mutations we may also get results we don’t want to know”
Stahel’s own focus is very much on identifying the right clinical questions and ensuring high-quality testing. He leads the European Thoracic Oncology Platform (ETOP), which in its Lungscape project is analysing a large cohort of NSCLC tumours for a panel of molecular characteristics such as ALK, and which is playing a part in the European EQA scheme, among other activities.
A regional network
One potential way forward with lung cancer is outlined by Thomas Zander, a lung oncologist at Cologne University Hospital in Germany, who attracted attention at this year’s ASCO with an abstract that described a regional screening network that has been set up for molecular testing of lung cancer patients at community hospitals in the Cologne-Bonn area. “The primary aim is to provide both well-established markers such as EGFR and ALK and also new diagnostics to community hospitals, so each lung cancer patient has the opportunity to know everything that is meaningful about their tumour,” says Zander. He calls the process ‘spreading’ – running assays on a panel of mutations, so that patients have opportunities to participate in trials and to obtain new drugs before approval.
“Take ALK – it is not yet in routine clinical testing or treatment with crizotinib, but there is a consensus that if you test and find it you should treat. In Germany, although you have to ask specifically for reimbursement, we have not had a problem in a single case, which is a good indication that the health community agrees it should be done. What we can do then is make drugs such as crizotinib available a year or so before approval.”
Crizotinib is being offered to patients via their primary oncologist, along with EGFR inhibitors, in Zander’s area. Other mutations being tested in Cologne include BRAF, KRAS, PIK3CA and ERBB2, with 1750 samples being tested so far, estimated at 60–70% of NSCLC cases in the region. Obtaining the right quality of material for lung cancer diagnostics is much more of problem than with colon cancer, he says, given the difficulty of gaining enough tumour cells from a lung biopsy.
“Obtaining the right quality of material for diagnostics is much more of problem with lung than with colon cancer”
Zander adds that the lung cancer testing represents a step-change in the number of assays being performed, using the array of technologies currently available. “We started with four or five assays, and we are already up to 14, and in a few years it could be 40,” he says. What is needed are technologies that ‘multiplex’ – measure simultaneously – the various mutations, and which home in only on those that are allowed to be searched for.
Zander agrees this is a challenge. “That’s the great problem with new gene sequencing technologies – soon it will be cheaper just to sequence everything, but for legal reasons we are not allowed to analyse anything else without asking the patient.” So far, assays at Cologne do focus only on key lung mutations, he says, while data hand-ling has not been an issue.
Cost is a major issue of course – outside of approved EGFR drugs there is no reimbursement for the often expensive diagnostics being done in Cologne, and Zander is reliant on grants.
National testing schemes
Meanwhile national schemes where centralisation is the theme are underway. Spain has taken early steps with demonstrating how national EGFR screening can work, as described in a much-cited paper from 2009 by Rafael Rosell and colleagues at the Spanish Lung Cancer Group (see Screening for epidermal growth factor receptor mutations in lung cancer; NEJM 361:958–967).
France probably has the most advanced national molecular profiling programme in Europe. Running for four years now, the French National Cancer Institute (INCa) and the Ministry of Health have set up a national network of 28 regional molecular genetics centres that carry out not just predictive tests such as for HER2, EGFR and KRAS status, and mutations in leukaemia and GIST that predict for response to Glivec (imatinib), but also diagnostics for factors such as chromosomal abnormalities in sarcomas and lymphomas, and prognostic tests to guide treatment in tumours such as neuroblastoma.
An idea of the scale is given in a paper by Frédérique Nowak and colleagues: in 2012, an estimated 40,500 patients will be diagnosed with colo-rectal cancer, of whom 17,500 will need to be tested for KRAS mutation status, which will be provided free of charge to patients and hospitals, with compensation to local pathologists who have to ship the tumour blocks to the regional centres. In 2011, more than 55,000 predictive tests were carried out in total, mainly in leukaemia, breast, colorectal and lung cancers.
The centres are also preparing the ground for the fast introduction of new agents, as Zander’s project is doing for lung cancer. A new-therapy programme is targeting biomarkers that are already in use in clinical trials. It was launched first for melanoma, lung and colorectal cancers – lung samples, for example, are being screened not just for EGFR but also for BRAF, KRAS, P13KCA, ALK and HER2, while an INCa-funded lung cancer database aims to make the most of linking molecular results with clinical and follow-up data.
Nowak and colleagues note too that “molecular tests performed on solid tumours are plagued by various sample-related and methodological problems” and that testing labs face a “permanent evolution of their daily practice”, which is challenging for those that are not research institutions. This is blurring the distinction between service provision and translational development, and needs the joint input of pathologists, molecular biologists and clinicians (for more on this see Tumour molecular profiling for deciding therapy – the French initiative, Nature Rev Clin Oncol 2012, 9:470–486).
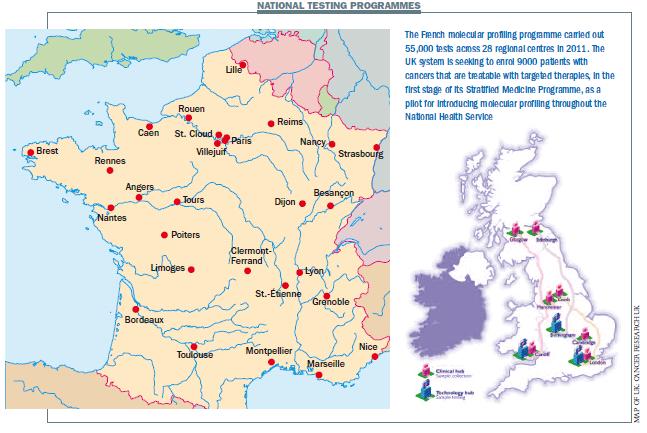 The UK also has an ambitious project in the Stratified Medicine Programme, headed by James Peach at the major charity, Cancer Research UK, with industry support. Many thousands of solid tumour tests are already being carried out in UK clinics, in particular EGFR and KRAS, but Peach says the project will show how they can be done collectively, mixing “say KRAS for colo-rectal cancer with BRAF and other markers to give a care choice to clinicians or accrual to a clinical study for researchers. We want to prove that standard tests such as KRAS can be linked to others in a single panel test,” he says.
The UK also has an ambitious project in the Stratified Medicine Programme, headed by James Peach at the major charity, Cancer Research UK, with industry support. Many thousands of solid tumour tests are already being carried out in UK clinics, in particular EGFR and KRAS, but Peach says the project will show how they can be done collectively, mixing “say KRAS for colo-rectal cancer with BRAF and other markers to give a care choice to clinicians or accrual to a clinical study for researchers. We want to prove that standard tests such as KRAS can be linked to others in a single panel test,” he says.
In the first phase of the programme, surplus material is being taken at hospitals with consent from about 9000 people with breast, colorectal, lung, prostate, ovary or melanoma tumours, which will be tested for about 20 mutations at three laboratories (over 2600 patients had enrolled in the programme by June 2012). The data will also be entered into a registry database alongside clinical outcomes. The key aim is to demonstrate to the UK’s NHS how quality-assured molecular testing can be done, with associated bioinformatics systems, at a low cost – the sum of £300 (€380) or less is mentioned for delivering a result that could have several markers.
“The key aim is to show how quality-assured molecular testing can be done, linked to bioinformatics, at a low cost”
Again, cost in the UK, as in other health services, is a sensitive issue – industry has stepped in to fund testing in the NHS and in other countries to support oncologists who were finding it hard to organise tests even for approved drugs. Merck Serono, for example, has been paying for KRAS tests to pave the way for Erbitux, while AstraZeneca initially funded EGFR tests for Iressa in the UK.
Peach says the UK is going through a similar learning curve to other countries in testing for mutations such as KRAS, and quality assessment schemes are currently underway from the UK National External Quality Assessment Service (NEQAS). A BRAF pilot for melanoma has also started. Networking with other countries, such as France, will be important, and also with industry.
While oncologists and pathologists try to digest this already challenging agenda, the information about cancer mutations just keeps on coming. In July this year, researchers at the Cancer Genome Atlas in the US published in Nature a ‘comprehensive molecular characterisation of colorectal cancer’, finding no fewer than 24 significant mutated genes. And in September, the Cancer Genome Atlas also found that half of squamous cell lung cancers, for which there are no current targeted therapies, have mutations that may be susceptible to current or new drugs – some of these no doubt will soon be added to Europe’s expanding molecular testing programmes.




Leave a Reply