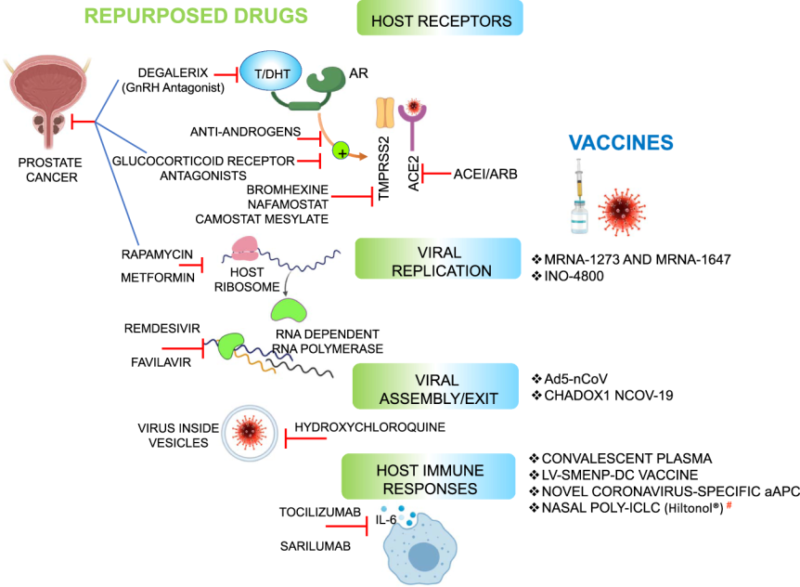
The overlapping biology identified between the molecular pathogenesis of COVID-19 and prostate cancer raises the possibility of repurposing drugs, including androgen deprivation therapy, for treating COVID-19, suggests a review in Nature Communications Biology, published 8 July. In the review the US authors additionally highlight the increased vulnerability of prostate cancer patients to COVID-19 and call for screening to be introduced.
“The particular vulnerability of older men to COVID-19 compels us to advocate for routine screening of SARS-CoV-2 infections in prostate cancer patients,” write Dimple Chakravarty and colleagues from Icahn School of Medicine, at Mount Sinai, New York.
The vulnerability of prostate cancer patients to COVID-19 is revealed by the authors own unpublished analysis, undertaken in the Mount Sinai Health System between March 1 2020 and April 26 2020. The study involved 9,648 COVID-19-positive patients, of whom 114 (2.2%) had been diagnosed with prostate cancer. Results revealed rates of intubation were greater for those diagnosed with prostate cancer than male patients with malignancies other than prostate cancer (25.4% vs 21.3%; P=0.02), and that mortality was greater for prostate cancer patients than male patients with other malignancies (23.7% vs 12.7%; P<0.01).
Accumulating evidence, write the authors, suggests similarities between risk factors for COVID-19 and prostate cancer. “Older age and comorbidities (hypertension, diabetes, obesity, and smoking) that adversely affect COVID-19 are also lethal for prostate cancer,” they write.
The authors draw attention to recent studies indicating that entry of SARS-CoV-2 (the virus causing COVID-19) into cells is through angiotensin-converting enzyme 2 (ACE2), and is also dependant on the serine protease activity of the TMPRSS2 gene (encoding for the transmembrane protease, serine 2). Studies indicate both ACE2 and TMPRSS2 may be under hormonal control, with higher levels of androgens signifying greater expression of these proteins, which could in turn increase vulnerability to COVID-19. Interestingly, an Italian study found that prostate cancer patients on androgen deprivation therapy were four times less likely to get infected with COVID-19 than prostate cancer patients not taking androgen deprivation therapy, and they were five times less likely to contract the disease compared to patients with other cancer types.
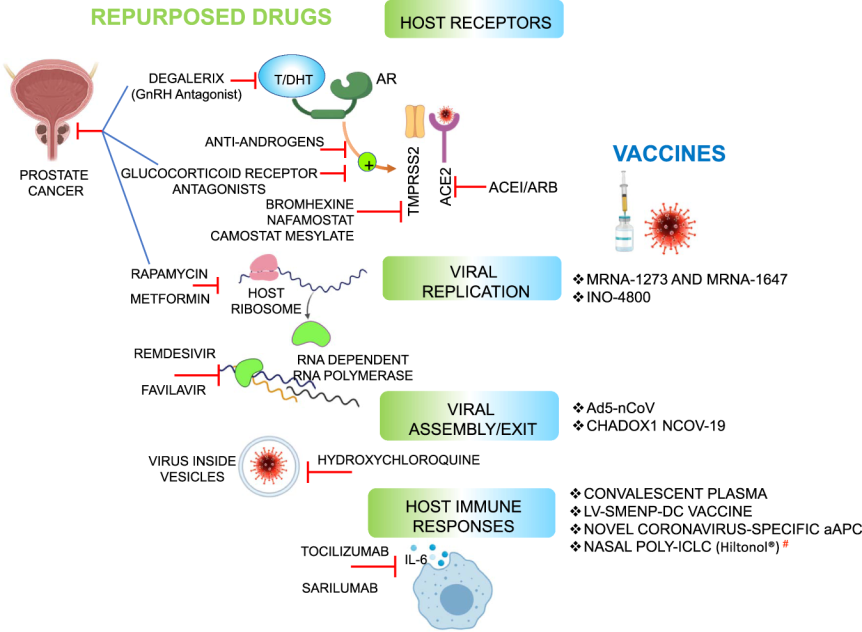
Source: D Chakravarty et al. Sex differences in SARS-CoV-2 infection rates and the potential link to prostate cancer. Commun Biol 3, 374 (2020). Reproduced under a Creative Commons licence 4.0
The interconnectivity between COVID-19 and prostate cancer raises the possibility that prostate cancer therapies could be repurposed for COVID-19 patients, including use of anti-androgens and androgen deprivation therapies (ADT), and furthermore that TMPRSS2 protease inhibitors might provide alternative therapies. Trials are currently underway exploring use of the antiandrogen bicalutamide on COVID-19 in Baltimore, Maryland, and more than nine different clinical trials are looking at blocking enzymatic activity of TMPRSS2.
In the review, the authors also consider the role of inflammation, with unpublished work by Chakravarty suggesting proinflammatory cytokines accelerate the progression of existing prostate cancer, with other studies showing that levels of IL-1 and IL-6 are associated with SARS-CoV-2 infection. “Systemic or tissue derived inflammation, during COVID-19, has the potential to accelerate pre-existing prostate cancer resulting in an aggressive phenotype and therefore represents a potential risk factor for prostate cancer patients,” write the authors.