Two ambitious data initiatives aimed at tracking a wide range of inequalities that contribute to big differences in the risk of dying from cancer were highlighted in the opening session of the 2022 European Cancer Summit, held in Brussels, November 15 and 16.
The first of these was the European Cancer Inequalities Registry, which is a flagship initiative of Europe’s Beating Cancer Plan. Managed by the EU Joint Research Centre under the auspices of the DG SANTE – the European Commission policy department for health and food safety – the newly established Cancer Inequalities Registry provides “sound and reliable data on cancer prevention and care to identify trends, disparities and inequalities between member states and regions”.
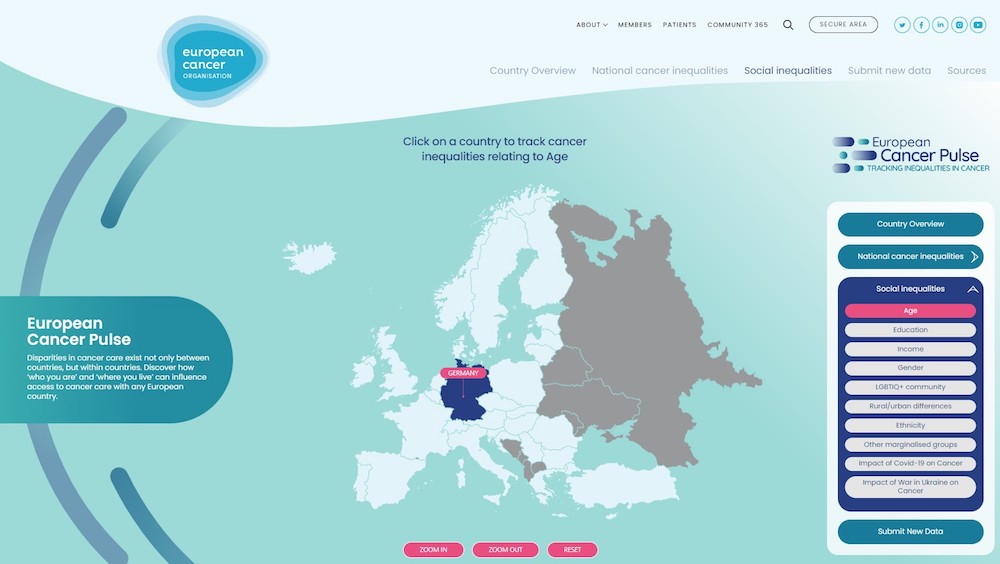
The second, the European Cancer Pulse, is an initiative launched by the European Cancer Organisation to complement the EU registry. This data gives access to a wider range of relevant data including, for example, data relating to quality of life or reintegration into the workforce, and levels of research activity, and relies heavily on crowd sourcing data from across the cancer community. Users can search for national level data, but they can also find data on inequalities within countries, eg by age, education, income, gender and ethnicity.
Both initiatives relate to the commitment in the Europe’s Beating Cancer Plan to “Reduce Cancer Inequalities Across the EU”. They aim to go beyond simply documenting disparities, to provide the data needed to understand and address the root causes of the disparities. This was clearly spelt out when the proposals for the Inequalities Registry were first published, as Flagship 9 of the Beating Cancer Plan: “Alongside regular qualitative assessments of the country-specific situation, the Registry will identify challenges and specific areas of action to guide investment and interventions at EU, national and regional level.”
Presenting the European Cancer Pulse at the European Cancer Summit, Mark Lawler, Professor of Digital Health at Queen’s University Belfast, and a board member of the European Cancer Organisation, stressed, “This is not an academic exercise. It is about identifying inequalities and then doing something about it. Follow the data, act on the data, trust the data, deliver on the data. “
Highlighting the “cancer crisis” facing Europe as a result of the Covid pandemic followed by a global economic downturn and the added pressures from the invasion of Ukraine, Lawler emphasized the importance of taking informed policy decisions based on data, not expert opinion. “Data eats opinion for lunch,” he said.
Caroline Berchet, a health economist at the OECD (Organisation for Economic Co-operation and Development) who works on the European Cancer Inequalities Registry explained the need for a wide range of data sets to understand – and address – the roots of inequalities in cancer burden and mortality, whether between countries, or between people from different socio-economic backgrounds or genders.
Headline inequalities include an almost doubled risk of dying from cancer in EU member states with the worst mortality rates compared with the best, and an 80% higher risk of dying from cancer among less educated men compared to their university educated counterparts (which falls to 30% among women).
Factors at play include exposure to risk (which in turn is determined by factors such as lifestyle as well as access to prevention information and opportunities); access to early detection (where factors such as organisation of screening programmes and awareness/health literacy play a role); and access to high quality cancer care (resources, workforce, training, organisation, guidelines, governance, and audit all play a role here, as do costs, Covid backlogs and more).
Policy makers need access to all these data, said Berchet, to inform what needs to be done to make serious inroads on reducing the inequalities.
Though the registry has made a great start, she said, “currently we only measure half the data that we need.” Important gaps include data on patient reported outcomes, workforce availability, spending on cancer care, and access to therapy, including authorisations, coverage, waiting times and affordability of cancer drugs.
The European Cancer Inequalities Registry and the European Cancer Pulse are both designed to present data in a way that is interactive and easy to visualise. Commenting in the panel discussion, Richard Sullivan, Director of the Institute of Cancer Policy at King’s College London, said the attention paid to presentation was essential to ensuring that the data does not just sit there, but gets used to inform policies and practices. “We all have a lot on our plate, so we need to be presented with information in a way that is actionable intelligence,” he said.
The European Cancer Summit is organised annually by the European Cancer Organisation, which brings together people from across the European cancer community to focus on areas where they can collaborate to improve the delivery of cancer prevention, detection and care. The issue of tackling cancer inequalities also featured in a number of other discussions conducted over the two-day event. This included a session around efforts to define, within different cancer settings, the outcomes that matter most to patients and ensure they are routinely measured and used to evaluate the quality of care as well as to improve the care of individual patients.
Also mentioned as a resource that could help harmonise quality of care was the Essential Requirements of Quality Cancer Care series of documents developed under the auspices of the European Cancer Organisation, by multiprofessional teams of experts drawn from across Europe, on a cancer by cancer basis.
The summit also touched upon what is widely seen as one of the more ambitious targets agreed in Europe’s Beating Cancer Plan in relation to reducing inequalities – namely the establishment of an EU Network linking recognised National Comprehensive Cancer Centres in every member state, with the aim of ensuring that 90% of European citizens have access to such centres by 2030.
Simon Oberst, who chairs the Accreditation and Designation board of the Organisation of European Cancer Institutes and co-chairs the European Cancer Organisation’s Quality Cancer Care Network, stressed the amount of work that would be required to meet this goal. He referred to ongoing work mapping the location of comprehensive cancer centres around Europe, and said that around 130 or even more such centres are envisaged, with a commitment for at least one in each member state.
While acknowledging the importance of ensuring sustainable funding for each one, he also stressed the importance of capacity building, twinning, and team projects to ensure that “those who are less well resourced in central and eastern Europe receive the required support to bring those centres up to higher quality standards for all the patients.” Integrating research into the activities of all the centres, he added, will be an essential part of raising standards of clinical care.