Spinal surgeon Bronek Boszczyk has said that training in complex surgery is like having to learn the violin during a full orchestral concert. The training revolves around closely supervised surgery on real patients in a real operating theatre – which means that not only is the pressure enormous, but also that there aren’t too many learning opportunities. Getting good takes a long, long time.
But in the past two decades, advances in technology have offered another option: detailed 3D simulations and online learning packages that not only provide plentiful practice but also tools for evaluation and developing skills. Surgeons and their organisations around the world are exploring this new way of training, based as much on the models of detailed simulation used by airline pilots as on traditional observation and supervision in the operating room.
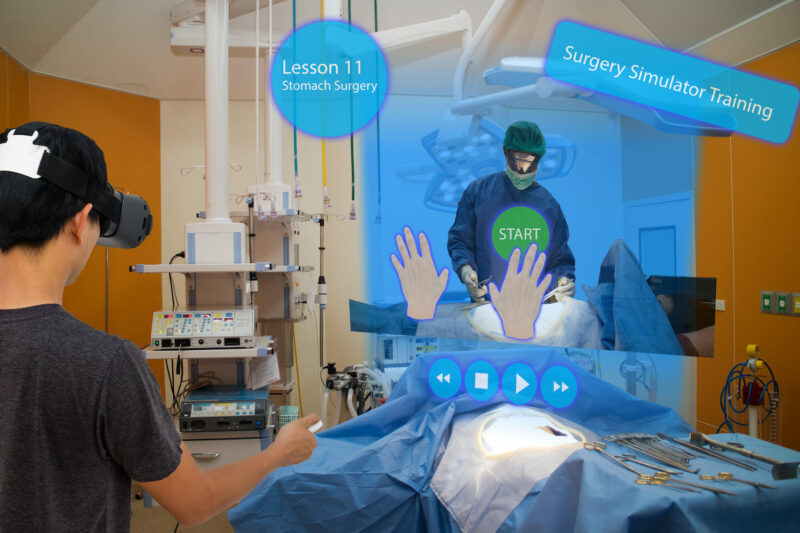
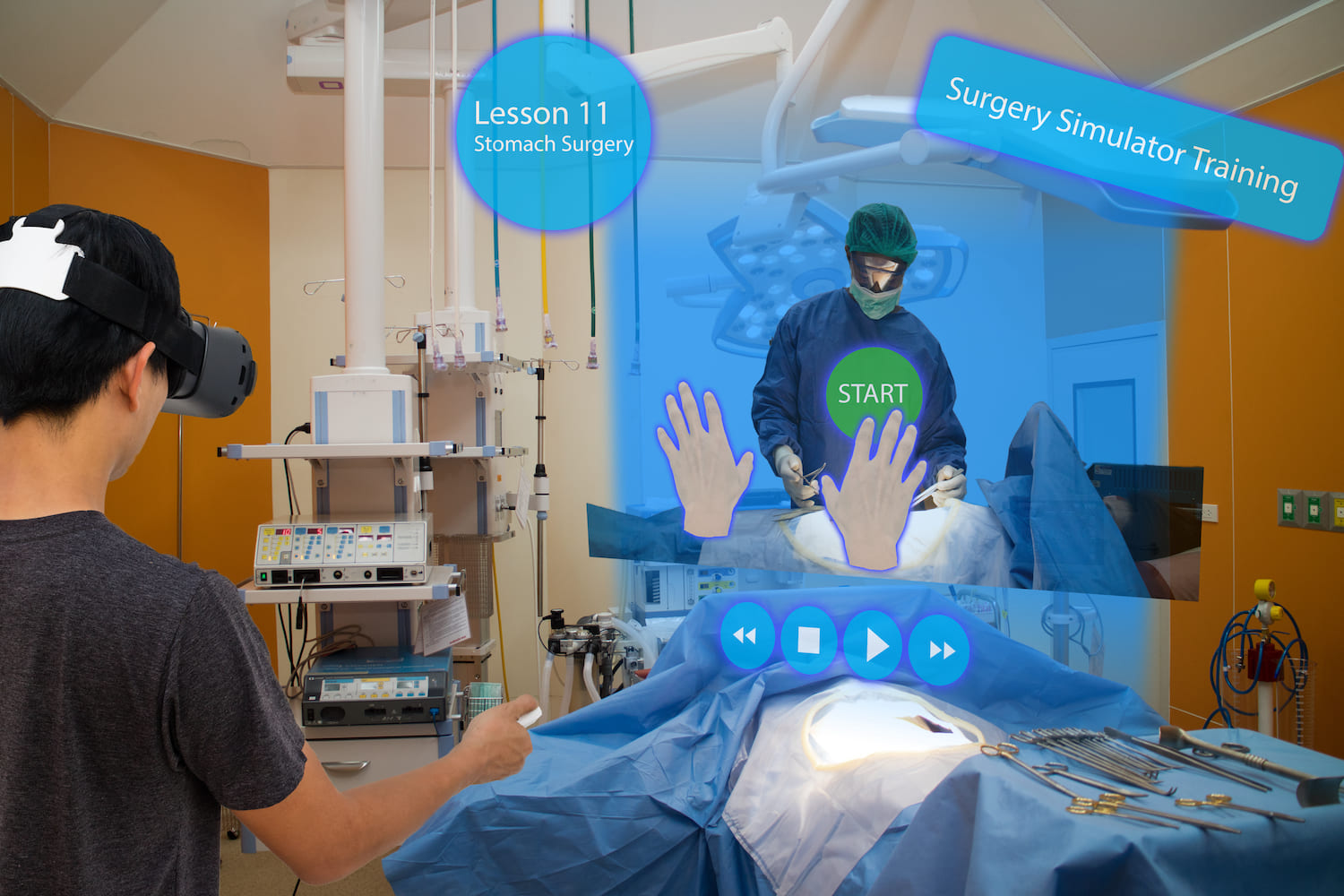
Dozens of tech companies are riding the wave of excitement, promoting virtual reality (VR) education platforms using VR headsets, haptic units (which recreate a sense of touch) and robotics, to provide a realistic replica of the operating theatre which the trainee can move around. Surgeons can download apps that enable them to review cases and learn new procedures. Holographic visors can be used to overlay scans and virtual anatomy onto models or real patients.
Interest exploded during the Covid-19 pandemic, when many elective procedures had to be postponed and access to the operating room became difficult because of social distancing. A 2021 German study into the role of VR in training surgical novices, in the light of the Covid pandemic, found VR simulator training improved the visual spatial ability of all 60 trainees studied.
In most countries, the pressures on both demand for and supply of cancer services that were exacerbated by the pandemic have persisted. The European Society of Surgical Oncology has been warning of the increasing demand for high-quality cancer surgery. In 2021, it wrote to European commissioners pointing out that, by 2030, 45 million surgical procedures will be needed worldwide. Yet currently, less than 25% of cancer patients globally actually receive safe, affordable, timely surgery.
According to Richard Sullivan, Co-Chair of the Lancet Oncology Commission on Global Cancer Surgery, which reported in 2015, “The failure to train more cancer surgeons and strengthen systems could result in as much as US$6.2 trillion in lost cumulative gross domestic product by 2030.”
We need to train more surgeons, more quickly, with no diminution of their skills. So is technology the way forward?
The question was posed by a Royal College of Surgeons (RCS) of England and the UK’s Association of Surgeons in Training in a comprehensive review published in August 2022. The Future of Surgery: Technology Enhanced Surgical Training Commission sprang from an awareness that, despite digital technologies being hailed as potentially transformative in surgery for decades, few advances had made a significant impact on surgical training. At the same time the technological ‘solutions’ market continues to expand.
Is technology the way forward for training surgeons?
Josh Burke, Chair of the Commission and Director for Education at the RCS England Innovation Hub, came away both dazzled by potential surgical training applications of digital technologies and humbled by the task that lies ahead to bring that potential to fruition – not just in the UK but across the world.
“I think one of the main things that the technologies afford is the potential to progress trainees through the current training pathways internationally at a more efficient rate and to a higher standard,” says Burke, a General Surgery Registrar in Manchester. The Commission hailed the ability of technologies to increase exposure to operating, allow trainees to learn while delivering effective patient care, and support assessment of trainee competency.
Each of those objectives is important, believes Burke. But it is the ability of tech to help in assessing competency, and direct trainees’ energies into areas requiring development, that particularly excites him. He explains that, historically, surgical training progression has been a numbers game, with the volume of procedures completed believed to indicate proficiency in performing it. In the real world, however, trainee surgeons develop skills at different rates. In addition, current competency workplace assessments are prone to being subjective rather than based on objective measures.
New tech provides the opportunity to be more “granular” and focused in training assessments, says Burke.
The ability of tech to help assess competency, and direct trainees’ energies into areas requiring development, is what excites him
“One of our report recommendations is that we could utilise some of the technology out there to adapt these work-based assessments,” he says. “It works really nicely. Some commercially available platforms can record an operation and break down the procedure into modular components using artificial intelligence. This could allow the surgeon trainer to assess those components in a more meaningful way after the operation has finished, and provide focused feedback on areas which require development.”
“Some of these programmes, particularly in robotics, generate metrics which if combined with surgeon wearables are a rich source of evidence about training competency – for example, how efficiently you use your instruments, your heart rate, your pupil dilation. The potential is incredibly exciting.”
Fulfilling the potential
But there are problems moving forward. These dominate the Commission report, and they apply to training programmes throughout Europe. One is that there is insufficient collaboration between technology providers and surgical training stakeholders to ensure that assessment of competence, benchmarking and training metrics are standardised and mapped to curricula.
Another centres on human resources. If there are insufficient doctors and nurses on the rotas, then it is impossible to create training environments that are conducive to taking advantage of all that technology can offer. “We must support, listen to and invest in the needs of our trainers, without whom any technology is merely a new, shiny object,” says Burke.
And, perhaps most frustratingly of all, is the lack of authoritative evidence supporting the use of the technologies, and with it any idea of genuine cost-effectiveness. Most of the research that does exist in the literature has been conducted by the manufacturers themselves.
“There remains no coordinated process to assess these technologies,” says the Royal College of Surgeons England report. “Regional investment in technology without proven efficacy is likely to be inefficient and costly and will increase variation in access to training that already exists.”
“I have yet to see a hard outcome indicating that a technology reduces the learning curve of a trainee or improves a patient outcome”
Burke adds: “There just aren’t any health economics impact assessments on training interventions like this. So although the educational outcomes look good superficially, and surgeons enjoy using them, I have yet to see a genuinely hard outcome indicating that a technology reduces the learning curve of a trainee, saves money or makes a patient outcome better.”
These issues are international, and the European Society of Surgical Oncology (ESSO) is in tune with the UK surgeons’ analysis about both the potential and failings of new technologies in surgical training.
Integrating new tech into training curricula
Jos van der Hage is Professor of Surgery and Professor of Medical Education at the University of Leiden and Co-Chair of the ESSO Education and Training Committee. Like Burke, he believes the priority is to ensure that all the technologies integrate into training curricula.
“What you need, and this is the current direction of research, is to identify the essential variables which are necessary to assess proficiency,” he says. “Then you need to standardise them and come up with an algorithm which is applicable to the educational curriculum.
“This is currently being done in the fields of laparoscopic and robot surgery, because these procedures are recorded and it’s easier to get data. People are looking at the movements of the instruments and comparing this in very skilled surgeons and novices performing the same surgical task. You can also assess spatial ability.”
Urology is currently leading the way, with the European Association of Urology having developed a training programme to assess junior urologists’ proficiency at robot-assisted prostatectomy. “This is definitely the way we are going in terms of assuring quality for patients,” says van der Hage.
“Simulated personalised training programmes maximise output and efficiency. That’s the expected benefit, but it will take some time”
At a time when many health services in Europe are struggling for lack of staff, new technologies definitely have a role in increasing cancer surgery capacity, he says. “To be able to meet societal demands in the future, you need to revolutionise your training programme. Simulated personalised training programmes maximise the output and maximise the efficiency. That’s the expected benefit, but it will take some time.”
What about the rest of the world?
It may benefit some countries sooner than others. Even if there were robust data demonstrating the benefits of high-tech training, and even if it could be standardised and integrated into curricula, there is the small question of cost.
Innovation does not tend to spread evenly. And ironically it is the places that stand to benefit most from increasing surgical training capacity where innovative training technologies are least affordable. The cost goes beyond purchasing the equipment.
“With the advent of these complex new technologies, the complexity of their management increases,” says van der Hage. “If you are an institution and you require a surgical robot, then you also get a training programme which is specially developed for this machine. So if you come from a country that doesn’t have the means to invest in these technologies, you cannot invest in the quality training either. Increased complexity using new technology always comes at a price.”
That pessimistic picture, however, might be offset by the example of some international projects that have demonstrated that new technologies can be used to train, supervise, and spread expertise among surgical oncologists in the geographical areas that need these skills most.
There is huge potential here, says van der Hage. “Trainees and residents in low- and middle-income countries can now get training from experienced colleagues in other countries by means of dedicated educational sites such as Incision [see end panel]. Also, if you are talking about hardware, with 3D glasses you can see in real time a surgical procedure which is not being performed in your hospital or your country.”
One project in Zambia is now proving that high-tech oncology surgery training can be achieved at a low cost. Researchers from the Institute of Cancer Policy at King’s College London, working with the University of Zambia and US university partners, used technology designed for home computer gaming to create a realistic VR surgical oncology simulation. The equipment was used to help prepare novice surgeons perform radical abdominal hysterectomy surgery procedures at the University Teaching Hospital, Women and Newborn in Lusaka. The total equipment cost was less than US$1,500.
“The question we asked was: Can low-cost VR surgery oncology simulation be developed and function well in lower resourced settings?” said Julie Torode, a visiting researcher at King’s College Hospital. “Well, the answer is: Yes we can.”
“The way we have been training in low- to middle-income countries is way too slow,” she said, speaking to a recent global webinar on technology in surgical training organised by the Global Surgery Foundation. “We need urgency and innovative ways to fill the gaps.”
The researchers chose radical abdominal hysterectomy for their trial because invasive cervical cancer is the number one cancer killer among women in most of sub-Saharan Africa. More than 50% of early-stage invasive cervical cancer can be cured with surgery alone, but radical abdominal hysterectomy is not available in most resource-constrained settings.
“We wanted to introduce new skills that could start saving women’s lives immediately,” said Torode, a cancer advocate who until recently worked as Deputy CEO and Director of Advocacy and Networks at the Union for International Cancer Control.
The system they developed was based on an off-the-shelf standard PC with a high-end graphics card and an Oculus Rift gaming headset. Training was delivered with a mentor at the trainee’s shoulder.
“It’s very easy to use,” explained Torode. “As in gaming, each student has their own dashboard, and they are able to see the breakdown of individual steps in the procedure and work towards personal goals for each of them.”
The system they developed was based on an off-the-shelf standard PC with a high-end graphics card and an Oculus Rift gaming headset
“Learning is rapid and all the students made improvements in accuracy across the training period, although the format seems to help some more than others. There’s a high retention of these skills, even when students rotated to other wards and then came back to the system.”
The research found that amount of training in virtual reality was highly predictive of accuracy in virtual reality. Continuing analysis of the data indicates that this, in turn, accelerates mastery of skills in a real operating room, but the final analysis has yet to be reported.
The project provides hope that the problem of cost is surmountable, and that there is a genuine prospect of technology helping build surgery capacity in resource-poor countries. Indeed, it may provide a direction for any country facing shortages of staff, tight training budgets and increasing demand.
What it also demonstrates – along with every other project using new digital technologies in the training of surgeons – is that no matter how shiny the devices are, they are still only tools, albeit sophisticated ones. The mentor at the shoulder, watching, advising, commenting on results, assessing, is going to remain at the core of surgery training.
Jos van der Hage says that, although the use of digital learning packages to assess theoretical skills is becoming well established, the routine use of technology to assess actual technical skills is still a way off. “Assessing technical skills virtually is really really difficult,” he says. So the continuing value that human trainers and assessors bring to the training process, and in building capacity and skills in health services, should not be underestimated.
“The technology is only as good as the people using it to train,” says Josh Burke. “There is some evidence to suggest that, when surgeons in training complete operations appropriately supervised, it can take longer.” As he points out, a lot of the learning isn’t just to do with a particular surgery or procedure. “There’s a lot of stuff that goes on around it which are intrinsic to building experience and competency. Throughout Europe, this training time is often underfunded and completely reliant on the goodwill of trainers and the hunger of those who want to learn.”
Top tech used in surgery training
Incision Academy
Interactive online courses and training materials for trainee surgeons and operating team members, to help them develop the competencies and skills. Content is delivered through an online, video-based academy designed to give everyone access to surgical education
Features:
- Accredited, video-based education and training
- Interactive 3D anatomy
- Test certification
https://www.youtube.com/watch?v=BjFkY1YJzkc
C-SATS Learning Community
A learning community for surgeons, using video capture of their robotic and laparoscopic operations and artificial intelligence to provide insights and measure skill development. Each step of a procedure is scored out of five using validated assessment tools for technical proficiency.
Features:
- Automatically segments steps of procedure for review
- Clinical insights provided by AI and fed into personal dashboard
- Trainers distil feedback to help trainees focus on areas that need development
- Surgical trainees can discuss procedures with peers and receive feedback from expert surgeons
- Surgeons in training can watch videos before performing a procedure for the first time
https://www.youtube.com/watch?v=s5vOCKd4igA
Intuitive’s SimNow
Uses virtual reality and video in a 3D high-definition interactive platform that replicates the experience of operating with a da Vinci robot for training purposes.
Features:
- Access to technical skills exercises, from basic to advanced training and practical modules
- Library of skills exercises and virtual reality surgical procedures
- Enables remote tracking and management of users’ performance in the simulation from any PC or smart device
https://www.youtube.com/watch?v=SNt_zmecta4
Fundamental VR
Offers a virtual reality education platform to support surgical learning in an immersive virtual surgical environment.
Features:
- Multimodal software platform that can be used on haptic units, 3D systems, headsets and robot arms
- Uses headsets to allow surgeons to walk through a procedure from any location
- Provides real-time feedback to users, who can repeat steps to gain a better understanding
- Trainer can virtually look over the trainee’s shoulder to watch the trainee perform a procedure remotely
- Dashboard summarises trainee’s answers to multiple choice questions asked during the procedure
https://www.youtube.com/watch?v=5OVNrbooals
Microsoft Hololens
Users wear a visor containing a display and an array of cameras and multiple sensors that pick up the surrounding room. Holograms are created by taking 2D video and turning it into a 3D version, overlaying the real environment. Using the visor, a holographic patient can be created in the physical room, or in a holographic hospital bed with surrounding machines.
Features:
- Enables trainees to participate in virtual ward rounds, seeing what the trainer sees and asking questions of the patient and trainer
- Surgeons can broadcast a procedure to trainees, enabling them to see a detailed view inside the body cavity
- Trainees can connect with other colleagues working on holograms