The Uganda Cancer Institute, set up in Kampala in 1967 as a centre for research and treatment of lymphoma, was one of the first cancer treatment centres in East Africa, and continues to play a leading role as a national and regional centre of excellence.
But it is entirely insufficient for the needs of a country with a population of 46 million, where rural communities still outnumber city dwellers by around four to one. This is one reason why, of the estimated 33,000 Ugandans who are diagnosed with cancer each year, only about 7,400 receive treatment – that’s less than one in every four. The Uganda Cancer Institute has become hopelessly congested. With a capacity of only 130 beds, those who arrive for treatment from all parts of the country often have to resort to sleeping on verandas, their mounds of possessions piled beside them. Many simply don’t come because the logistics of travel and where to stay are so difficult.
In an effort to improve access to cancer care across the country, the government has committed to setting up regional cancer centres. In November 2023 the Uganda Cancer Institute opened the Northern Region Cancer Center, in Gulu City – almost 350 km north of Kampala. This follows the establishment of the Western Region Cancer Center in Mbara – around 270 km to the west, which is already operational. An Eastern Region Cancer Center is due to open in Mbale – 225 km east of Kampala – next year.
The hope and expectation is that these regional centres will not only decongest the Uganda Cancer Institute in Kampala (UCI Kampala), but will also enable prompt treatment, better community awareness and earlier detection. “Once services are extended to the regions, the time spent for someone with suspected cancer to get a proper diagnosis will be shortened,” says Christine Namulindwa, Public Relations Officer at the Uganda Cancer Institute.
“Cancer has no boundaries,” says Henry Ddungu, Senior Consultant Haematologist and head of the division of medical oncology and haematology at UCI Kampala. “If you have decentralisation of cancer services, at least the basic services can get to the people. Even continuity of care comes easier if someone can access a centre that is near.”
Historically, around 85% of Ugandans have had to travel significant distances to access services, facing challenges of travel, accommodation and paying for sustenance during their treatment.
Policy makers and clinicians are now optimistic that the roll-out of regional cancer centres, which will provide services largely free of charge, will alleviate many of these access problems. But there are concerns about the limitations of the initiative, in particular regarding its long-term sustainability. Funding for the Northern Region Cancer Center in Gulu came from a loan agreement between the Government of Uganda and Austria totalling €7.5 million. But this was designed to cover the costs of construction and equipment. The question is: where will the funding for running and treatment costs come from?
The Uganda Cancer Institute receives funding direct from the Uganda government. Most of the costs of treatment are covered, though patients are often required to pay some ‘top up’ fees. A private wing is available for patients who can afford it.
Ddungu says that funding through a national insurance system might be an option in the future, but the high cost of cancer care means that premiums might not be affordable. He has suggested exploring business strategies and philanthropic contributions as potential avenues to sustain these vital programmes. “It’s essential to instil a sense of philanthropy within our community,” he says.
As things stand, resourcing issues are limiting the range of treatments available at the regional centres. The Northern Regional Center in Gulu, for example, is well-equipped to offer surgical procedures, chemotherapy, and CT scans, but radiotherapy is not available.
Oncologists at the Uganda Cancer Institute are proposing a temporary way forward, which would involve patients receiving their chemotherapy treatment in regional centres, then being transferred to UCI Kampala for radiotherapy, if required. This approach is considered less challenging than requiring individuals living far from Kampala to make that journey for the combined chemotherapy and radiation. Ddungu says that scientific evidence needs to be gathered to support this treatment approach. “The ultimate goal is to make radiation available at regional centres,” he says.
Training up new cades of highly specialised professionals will also be key to extend high quality care to the regional centres, adds Ddungu. The Government is working with the Uganda Cancer Institute to achieve this, through fellowship programmes. The objective is to enable individuals to specialise, by undergoing a two-year, hands-on training programme immediately after obtaining their Master’s degree.
As a regional centre of excellence, this training role is one that the Uganda Cancer Institute has played for a long time within the wider East Africa Region, often in collaboration with international partners.
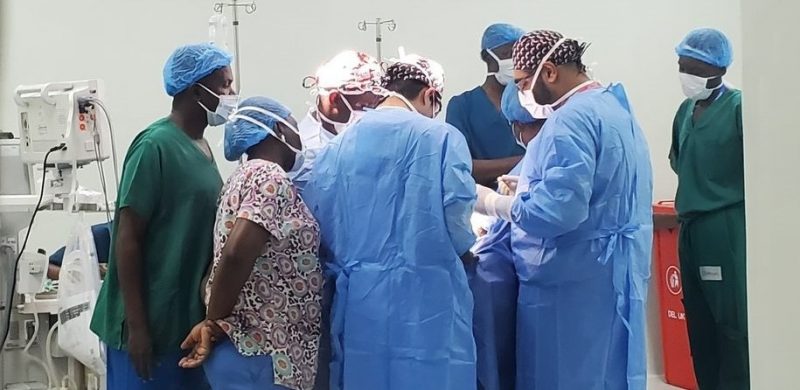
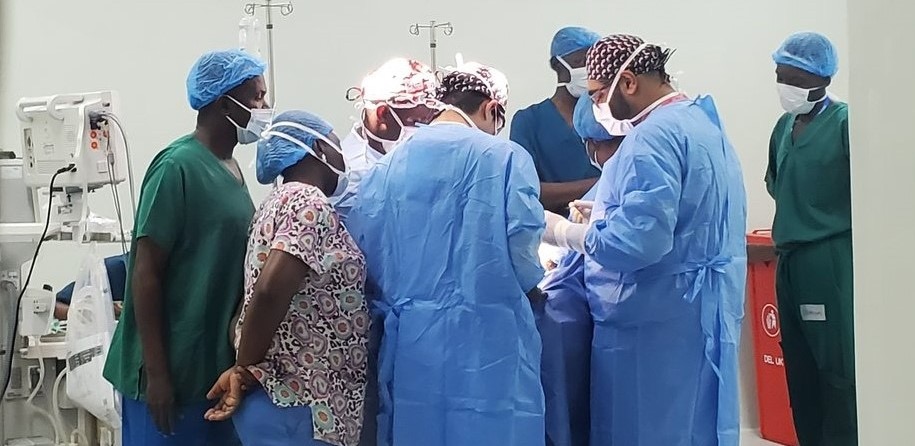
One such partnership is with the US Head and Neck Outreach organisation, which provides training to young oncologists in Uganda in diagnostics and treatment of head and neck cancers. The opening illustration shows an operation being carried out in November 2023, at the newly opened Northern Region Cancer Center in Gulu, as part of a week-long head and neck surgery training event.
Picture credit: Patrick Uma ©2023